Department of Pathology Updates Vol 3(2)
By Jeffrey Myers | December 31 2017Teammates,
Welcome to a year-end edition of DOP Updates, an email sent to members of our Department of Pathology (DOP) team and others to focus on issues, events, and topics of common interest. If there is something that you would like to share with your colleagues and co-workers, please send me an email and I’ll be sure to include it next time. As with all previous editions, I have also attached a PDF of this to preserve formatting across platforms.
Building a Sacred Place (by Risa Tisdale VanDerAue IN: Linda R. Larin (Editor). Inspired to Change. Improving Patient Care One Story at a Time. Health Administration Press. Chicago. 2014)
Ten years ago, a cardiac tumor brought me into the hospital. What I found in this place of healing was a sacred space, built by people who were moved by their own hearts to mend the patients’ bodies and souls and to care for their entire families. Let me share my story with you.
At age 29 and pregnant with my second child, I went into fulminant heart failure and was air-lifted to an academic medical center. An atrial myxoma was making it impossible for me to breathe. The tumor was successfully removed, but my system began to fail, requiring me to be placed on ECMO (extracorporeal membrane oxygenation) life support. While unconscious and sustained by machines and prayers, I delivered my stillborn daughter. In her death, she bequeathed the gift of life. Had I not been pregnant, my tumor would not have been discovered until it was too late. My precious child bestowed her soul to me and to her sister, who at two years old needed her mom.
 When I awoke about six weeks later, I found that I was connected to another machine – an LVAD (left ventricular assist device) – to help my heart pump blood. I was told that this apparatus would let my heart rest while I waited for a transplant. On Christmas Day in 2003, with my toddler sitting on my lap, I was wheeled out of the hospital and sent home with a backpack containing heavy batteries and a constantly whirring pump. Sometimes I joke that I used every department the hospital had to offer except Orthopedics, but that is not an exaggeration. I am alive and healthy today because of the innovative technology created through modern health science. My inspiration for telling my story, however, is not the machines but the humanity my family and I experienced during my stay. Yes, I was on many life support systems, but not all of them were plugged into a wall socket. The staff – from the maintenance crew to the surgeons – were my spiritual life support, keeping me alive and my family comforted and reassured with their pure gestures of compassion, kindness, and concern.
When I awoke about six weeks later, I found that I was connected to another machine – an LVAD (left ventricular assist device) – to help my heart pump blood. I was told that this apparatus would let my heart rest while I waited for a transplant. On Christmas Day in 2003, with my toddler sitting on my lap, I was wheeled out of the hospital and sent home with a backpack containing heavy batteries and a constantly whirring pump. Sometimes I joke that I used every department the hospital had to offer except Orthopedics, but that is not an exaggeration. I am alive and healthy today because of the innovative technology created through modern health science. My inspiration for telling my story, however, is not the machines but the humanity my family and I experienced during my stay. Yes, I was on many life support systems, but not all of them were plugged into a wall socket. The staff – from the maintenance crew to the surgeons – were my spiritual life support, keeping me alive and my family comforted and reassured with their pure gestures of compassion, kindness, and concern.
My parents and sister moved into the waiting room outside the cardiac ICU so that I was never alone. The ICU staff not only supported their presence but also encouraged it. My family ate, slept, and prayed near my bedside, and the waiting room became something of a sanctuary for those who came to visit me. They filled the room with food and drink, blankets and pillows, and love and support. A kind housekeeping employee checked in on my family, by name, every day. He would only clean the room when it caused the least amount of disruption to my family and not when it was most convenient for him. My father offered him a small gratuity to thank him for his patience, but the man kindly declined, saying he was only doing his job. But for us, his occupation was not just janitorial but also as a healer; he healed our souls with his deeds just as the surgeons fixed my heart with their scalpels.
During my lengthy stay in the hospital, my family and I encountered hundreds of doctors, nurses, and support staff who treated us with dignity, respect, and compassion. Many of them stayed well past the end of their shifts to sit with us and to offer comfort and support. Doctors from all departments visited, sometimes after 14-hour surgeries, to inquire about my condition and how my family was holding up. Nursing assistants made special accommodations for my young daughter to spend time with me; they covered my LVAD and silenced the alarms so she would not become frightened.
At a particularly dire moment, a young man mopping the floors found my sister in the basement of the hospital, consumed with grief and fear, weeping alone. He stopped what he was doing, bought her a soda from the vending machine, and asked what he could do to help. A soda may be a small gesture, but that night it was a grand, unforgettable gift to my sister. It was an unsolicited donation from a compassionate heart who reached out to a soul in need – a sacred gift, indeed.
Fortunately, I did not end up needing a transplant; my heart healed on its own, and in February 2004, my LVAD was removed. I was one of the lucky ones. When the doctor signed my final discharge papers, I was not quite sure what to do. He told me to go home and live my life. With my daughter, now almost 12 years old, by my side, I have done just that. I was given a chance for a full life made possible through innumerable gifts from so many willing, loving, and dedicated people.
I thought that my family and I were the only recipients of this great gift of healing and recovery, but I was wrong. A heart transplant coordinator, who came with me to all of my tests and procedures, shared with me that my case had touched her. A few years earlier, another young person with a similar condition did not survive, and the staff was devastated. My recovery and my discharge on Christmas Day turned out to be a gift to the staff, to each and every person who we had come into contact with during my long ordeal. It reinvigorated them and reinforced their dedication to helping save the lives of others. It reminded them what they do makes a difference, that who they are matters, and that their sacrifices are valuable.
In the years since my discharge, I have been asked on many occasions to tell my story. When the new cardiovascular center was being designed and built, I sat on a panel to research what patients would like to see in the facility. When the building was completed, I spoke at staff training sessions to help prepare the staff for their transition to the new center. In truth, the medical details of my illness have begun to fade from my memory, and for that I am grateful. I no longer remember the number of heart catheterizations I had or the number of chest tubes inserted into me. But I vividly remember the compassion, love, and kindness my family and I received. My heart healed, in part, because of the sacred gifts from those whose hearts were moved to be so caring for us.
Servant leadership and knowing your why
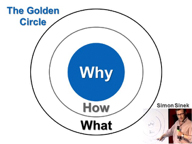 Great organizations differ from good ones in many important ways. Some would argue that chief among them is a clearly articulated and deeply embedded sense of purpose. Simon Sinek maintains that greatness is rooted in knowing why you do what you do as opposed to focusing solely on what you do and how you do it. It is the difference between knowing what happens in our laboratories and how, and instead doing all of this knowing at your core that we are in the business of transforming the experience of patients and families from a laboratory platform deeply rooted in a legacy of world-class care, a generations-deep commitment to educating those who will care for us, and the discipline to invest in the discoveries that will change for the better how those we’ve not yet met will experience health and disease in the future. That is our why. We do what we do because we believe that we can change the world or at least a piece of it.
Great organizations differ from good ones in many important ways. Some would argue that chief among them is a clearly articulated and deeply embedded sense of purpose. Simon Sinek maintains that greatness is rooted in knowing why you do what you do as opposed to focusing solely on what you do and how you do it. It is the difference between knowing what happens in our laboratories and how, and instead doing all of this knowing at your core that we are in the business of transforming the experience of patients and families from a laboratory platform deeply rooted in a legacy of world-class care, a generations-deep commitment to educating those who will care for us, and the discipline to invest in the discoveries that will change for the better how those we’ve not yet met will experience health and disease in the future. That is our why. We do what we do because we believe that we can change the world or at least a piece of it.
Success in changing the world brings with it an insatiable appetite for leadership. Not leadership as traditionally defined by positions of authority, but instead leadership as walked out every day by those at all levels of our department and organization who step forward to understand and solve problems while others are content with things as they are. The capacity to lead resides in all of us and hinges on a willingness to step beyond the limits of our own comfort with the determination to deliver us to a better place in which compassion and kindness are our guides.
I was thinking about these things when a friend shared with me a poem now almost 50 years old, The Paradoxical Commandments, written by Kent Keith to offer guidance to student leaders when he was only 19 years old. It seems to me relevant today as we care for others, inspired by stories like Risa VanDerAue’s whose journey was touched not only by her nurses and doctors but also by “pure gestures of compassion, kindness, and concern” from staff who volunteered a soda (“a grand, unforgettable gift”) to her sister in a time of need, and another who became a healer by prioritizing her family’s interests above his own schedule. And as a consequence, the world changed. Perhaps these simple suggestions from Kent Keith will bring us one step closer to transformation in 2018.
The Paradoxical CommandmentsKent M. Keith |
|
|
|
Auld lang syne
 2017 has been a remarkable year for our Department of Pathology across all of our missions. In our clinical domain, we’ve lost talented faculty and staff to retirement, end of life, and career transitions of the sort that are the hallmark of places to which others turn for the talent important to achieving their own dreams and aspirations. And in response, we have continued to recruit the very best and brightest at an astounding rate, testimony to the strength and appeal of a place that prides itself on the rewards realized from working together to transform the experience of patients and their families, those who care for them, and one another. I was once told that an ability to recruit highly talented faculty, staff, trainees, and students is a key metric when it comes to judging the strength of any academic enterprise, and on that score, I suspect we remain 2nd to none!
2017 has been a remarkable year for our Department of Pathology across all of our missions. In our clinical domain, we’ve lost talented faculty and staff to retirement, end of life, and career transitions of the sort that are the hallmark of places to which others turn for the talent important to achieving their own dreams and aspirations. And in response, we have continued to recruit the very best and brightest at an astounding rate, testimony to the strength and appeal of a place that prides itself on the rewards realized from working together to transform the experience of patients and their families, those who care for them, and one another. I was once told that an ability to recruit highly talented faculty, staff, trainees, and students is a key metric when it comes to judging the strength of any academic enterprise, and on that score, I suspect we remain 2nd to none!
In the last year, we’ve seen our Pathology Informatics group tackle enormous opportunities and challenges in a way that others can only envy. Accomplishments include continued evolution of our increasingly robust laboratory information system (LIS). They have also worked with colleagues in our Division of Quality and Health Improvement (DQHI) to create novel solutions in support of our Patient Assets Management Initiative (PAMI). In partnership with Lloyd Stoolman, Josh Jacques, and Peter Ouillette they have supported new digital solutions that will position us for success in our relocation and renovation project.
Our clinical laboratories, in collaboration with DQHI, have maintained their commitment to doing better tomorrow the things we already do well today through continuous improvement and a passionate belief in what’s possible. Our collaborative investments in quality were on review in another extremely successful visit by peers representing the College of American Pathology (CAP), resulting in re-accreditation of our laboratories.
In addition to their support of compliance and leading our project to revolutionize our ability to track the precious patient assets entrusted to our care, DQHI faculty and staff are working with others across departments and schools to create new value by doing only the right tests for the right patients at the right time through more appropriate utilization of laboratory resources. And our Patient and Family Advisory Council (PFAC) celebrated its first birthday as it continues to work directly with patients and families to more fully understand our opportunities to transform their experience of care.
MLabs continued to extend our ability to touch the lives of patients who live beyond the historical reach of own health system, acquiring new clients from coast-to-coast while also supporting regional growth strategies for Michigan Medicine including an agreement signed only this month with MidMichigan Health to become their primary reference laboratory provider. Restructuring combined with a focus on strategy has positioned us to succeed as a premier reference laboratory provider dedicated to building relationships focused on improving the health of patients and families everywhere. And we do this by offering access to the talented students, trainees, staff and faculty who are most responsible for our collective successes . . . Mlabs is YOU!
And 2017 saw BIG PROGRESS in our Pathology Relocation and Renovation (PRR) project that will see a large part of our clinical operations relocate to the North Campus Research Center (NCRC) this summer. More than anything we’ve done together, this project illustrates the power of entrusting those who do the work with designing our future. It is impossible to overstate the power of co-locating so many of our clinical operations, learners, staff, and faculty when it comes to our innovative capacity. Whatever the challenges of providing care at a distance, I have never been more confident in our ability to change the way we care for others from our redesigned laboratory and non-laboratory spaces.
As great as our accomplishments in 2017, there is every reason to believe that 2018 will be another year in which we will have much to celebrate . . . HAPPY NEW YEAR!
That’s the news for the moment. Thank you for all that each and every one of you has done and continues to do on behalf of our patients and their families, whether they are those who look to us for comfort today, or are instead the patients we’ve not yet met who will be the beneficiaries of our commitment to educating those who will follow us and the discoveries with the potential to change the future of healthcare. There is much to be done, but nowhere is there a team more powerful than this one when it comes to the rewards realized from working together to transform the experience of patients, their families, those who care for them, and one another. And as we build this sacred place, let’s be careful out there . . .
 ON THE COVER
ON THE COVER
 ON THE COVER
ON THE COVER
 ON THE COVER
ON THE COVER
 ON THE COVER
ON THE COVER
 ON THE COVER
ON THE COVER
 ON THE COVER
ON THE COVER
 ON THE COVER
ON THE COVER
 ON THE COVER
ON THE COVER
 ON THE COVER
ON THE COVER
 ON THE COVER
ON THE COVER
 ON THE COVER
ON THE COVER
