

By Elizabeth Walker | Photography by Dustin Johnston | 25 July
A giant mural depicting a cheery forest of tree houses covers a wall in the C.S. Mott Children’s and Women’s Hospital (C&W) outpatient blood draw station. The artwork serves as a soothing distraction for waiting pediatric patients and their families.
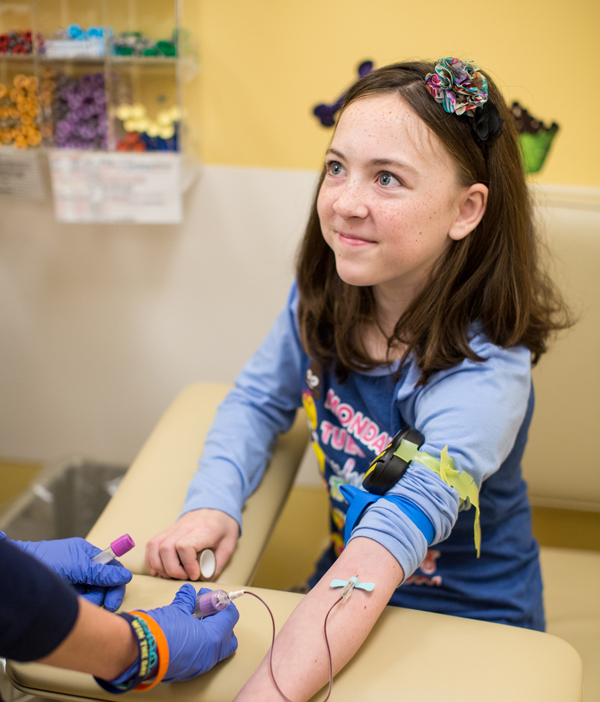
Blood draws account for a significant component of the care provided at C&W. While the facilities are bright and comfortable, the Department of Pathology’s Manger of Specimen Procurement, Harry Neusius, SM (ASCP) MBA explains that there’s still a clinical air in the environment that can be significant for pediatric patients. “There is a need to calm the anxiety associated with needle-sticks,” says Neusius. “It’s not just a blood draw. There’s more to it than getting access to a vein.”
Phlebotomists are the face of the laboratory. They’re on the front lines, having an opportunity to influence the patient experience with each poke.
In an effort to ease anxieties on both sides of the experience, a two-year study was conducted to look at phlebotomists’ self-reported knowledge, training, stress levels, and the techniques used with their patients during pediatric blood draws. The study also gathered feedback from the patients and their parents.
What resulted is a six-part care plan for pokes and procedures, known as the Poke Plan.
Part one focuses on gathering information from patients and their caregivers. “We wanted to give the child a voice, to ask how they want to have their blood drawn. Did they want to lie down? Be held by a parent?” explains Associate Supervisor of Inpatient Phlebotomy, Cindy Straub. In addition to positioning, questions about helpful distractions, use of comfort measures, and whether or not the patient would like to watch are asked.
The answers are then shared with phlebotomists via an electronic version in the patient’s chart and hard copies posted outside of patient rooms on the floors. Julie Piazza, MS, CCLS who was the primary investigator of the study and is a Child Life Specialist, says that families asked for a copy that they could keep. A version in the form of a paper passport was developed for patients. There are also plans to possibly develop an app for the future.
The second part of the plan involves using distraction to help children feel less anxious before their blood draw and to recover more quickly after. Piazza explains that pre-procedure interactions with the child and family are key. Building relationships starts with the phlebotomist introducing him or herself and then gravitating toward conversations that are common and comfortable.
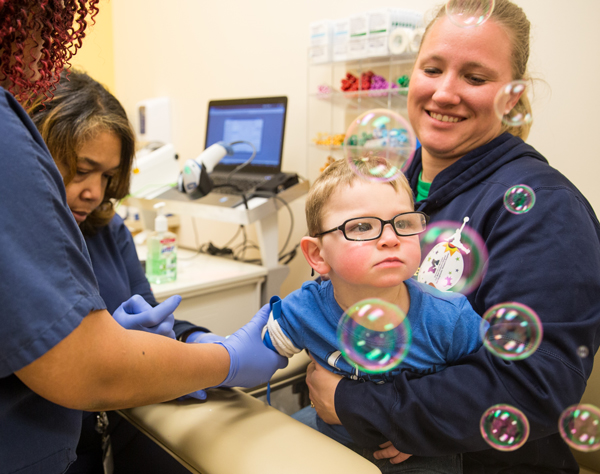 Children may also benefit from counting, singing, blowing bubbles, reading a book, or using an iPad. Child Life Specialists are on call to bring toys and books as requested.
Children may also benefit from counting, singing, blowing bubbles, reading a book, or using an iPad. Child Life Specialists are on call to bring toys and books as requested.
Patient positioning is the key to step three. Positions with some physical contact between parent and child allow each a sense of control.
While some parents may choose not to participate in the poke or procedure, those who do are encouraged to act as coaches before, during, and after a poke in step four. Parents should be aware of how their reaction to the situation may influence their child. Speaking in a calm, soothing matter and acknowledging that it’s a difficult situation can be very helpful to a crying child.
Choosing the “best words” for the situation is step five. The rhetoric of the blood draw is an important component of the patient experience. Phlebotomists are encouraged to use “kid’s speak” for medical terms. Referring to an alcohol prep pad as a “tiny washcloth”, a tourniquet as “a tight hug for your arm”, and veins as “tiny tunnels that run all through your body”, can lessen a child’s fear.
 Finally, phlebotomists may use a topical numbing cream when accessing a patient’s chest port or devices may be used to draw a child’s attention away from the site of draw. A popular device is Buzzy®, which provides vibration in the form of a friendly looking bumblebee.
Finally, phlebotomists may use a topical numbing cream when accessing a patient’s chest port or devices may be used to draw a child’s attention away from the site of draw. A popular device is Buzzy®, which provides vibration in the form of a friendly looking bumblebee.
All of these steps allow phlebotomists to be successful in interacting with their patients and empower parents with inclusion in their children’s treatment. “We found in this journey,” says Piazza, “that the concern we have for their family member’s comfort was key in patient satisfaction.”
It’s more than just a blood draw and the willingness of all stakeholders to participate in research improves safety, quality, and comfort outcomes.
 ON THE COVER
ON THE COVER
Breast team reviewing a patient's slide. (From left to right) Ghassan Allo, Fellow; Laura Walters, Clinical Lecturer; Celina Kleer, Professor. See Article 2014Department Chair |

newsletter
INSIDE PATHOLOGYAbout Our NewsletterInside Pathology is an newsletter published by the Chairman's Office to bring news and updates from inside the department's research and to become familiar with those leading it. It is our hope that those who read it will enjoy hearing about those new and familiar, and perhaps help in furthering our research. CONTENTS
|
 ON THE COVER
ON THE COVER
Autopsy Technician draws blood while working in the Wayne County morgue. See Article 2016Department Chair |

newsletter
INSIDE PATHOLOGYAbout Our NewsletterInside Pathology is an newsletter published by the Chairman's Office to bring news and updates from inside the department's research and to become familiar with those leading it. It is our hope that those who read it will enjoy hearing about those new and familiar, and perhaps help in furthering our research. CONTENTS
|
 ON THE COVER
ON THE COVER
Dr. Sriram Venneti, MD, PhD and Postdoctoral Fellow, Chan Chung, PhD investigate pediatric brain cancer. See Article 2017Department Chair |

newsletter
INSIDE PATHOLOGYAbout Our NewsletterInside Pathology is an newsletter published by the Chairman's Office to bring news and updates from inside the department's research and to become familiar with those leading it. It is our hope that those who read it will enjoy hearing about those new and familiar, and perhaps help in furthering our research. CONTENTS
|
 ON THE COVER
ON THE COVER
Director of the Neuropathology Fellowship, Dr. Sandra Camelo-Piragua serves on the Patient and Family Advisory Council. 2018Department Chair |

newsletter
INSIDE PATHOLOGYAbout Our NewsletterInside Pathology is an newsletter published by the Chairman's Office to bring news and updates from inside the department's research and to become familiar with those leading it. It is our hope that those who read it will enjoy hearing about those new and familiar, and perhaps help in furthering our research. CONTENTS
|
 ON THE COVER
ON THE COVER
Residents Ashley Bradt (left) and William Perry work at a multi-headed scope in our new facility. 2019Department Chair |

newsletter
INSIDE PATHOLOGYAbout Our NewsletterInside Pathology is an newsletter published by the Chairman's Office to bring news and updates from inside the department's research and to become familiar with those leading it. It is our hope that those who read it will enjoy hearing about those new and familiar, and perhaps help in furthering our research. CONTENTS
|
 ON THE COVER
ON THE COVER
Dr. Kristine Konopka (right) instructing residents while using a multi-headed microscope. 2020Department Chair |

newsletter
INSIDE PATHOLOGYAbout Our NewsletterInside Pathology is an newsletter published by the Chairman's Office to bring news and updates from inside the department's research and to become familiar with those leading it. It is our hope that those who read it will enjoy hearing about those new and familiar, and perhaps help in furthering our research. CONTENTS
|
 ON THE COVER
ON THE COVER
Patient specimens poised for COVID-19 PCR testing. 2021Department Chair |

newsletter
INSIDE PATHOLOGYAbout Our NewsletterInside Pathology is an newsletter published by the Chairman's Office to bring news and updates from inside the department's research and to become familiar with those leading it. It is our hope that those who read it will enjoy hearing about those new and familiar, and perhaps help in furthering our research. CONTENTS
|
 ON THE COVER
ON THE COVER
Dr. Pantanowitz demonstrates using machine learning in analyzing slides. 2022Department Chair |

newsletter
INSIDE PATHOLOGYAbout Our NewsletterInside Pathology is an newsletter published by the Chairman's Office to bring news and updates from inside the department's research and to become familiar with those leading it. It is our hope that those who read it will enjoy hearing about those new and familiar, and perhaps help in furthering our research. CONTENTS
|
 ON THE COVER
ON THE COVER
(Left to Right) Drs. Angela Wu, Laura Lamps, and Maria Westerhoff. 2023Department Chair |

newsletter
INSIDE PATHOLOGYAbout Our NewsletterInside Pathology is an newsletter published by the Chairman's Office to bring news and updates from inside the department's research and to become familiar with those leading it. It is our hope that those who read it will enjoy hearing about those new and familiar, and perhaps help in furthering our research. CONTENTS
|
 ON THE COVER
ON THE COVER
Illustration representing the various machines and processing used within our labs. 2024Department Chair |

newsletter
INSIDE PATHOLOGYAbout Our NewsletterInside Pathology is an newsletter published by the Chairman's Office to bring news and updates from inside the department's research and to become familiar with those leading it. It is our hope that those who read it will enjoy hearing about those new and familiar, and perhaps help in furthering our research. CONTENTS
|
 ON THE COVER
ON THE COVER
Rendering of the D. Dan and Betty Khn Health Care Pavilion. Credit: HOK 2025Department Chair |

newsletter
INSIDE PATHOLOGYAbout Our NewsletterInside Pathology is an newsletter published by the Chairman's Office to bring news and updates from inside the department's research and to become familiar with those leading it. It is our hope that those who read it will enjoy hearing about those new and familiar, and perhaps help in furthering our research. CONTENTS
|

MLabs, established in 1985, functions as a portal to provide pathologists, hospitals. and other reference laboratories access to the faculty, staff and laboratories of the University of Michigan Health System’s Department of Pathology. MLabs is a recognized leader for advanced molecular diagnostic testing, helpful consultants and exceptional customer service.