Research Surrounding H3K27M-mutant diffuse midline glioma in COVID-19 Published
By Camren Clouthier | July 7 2020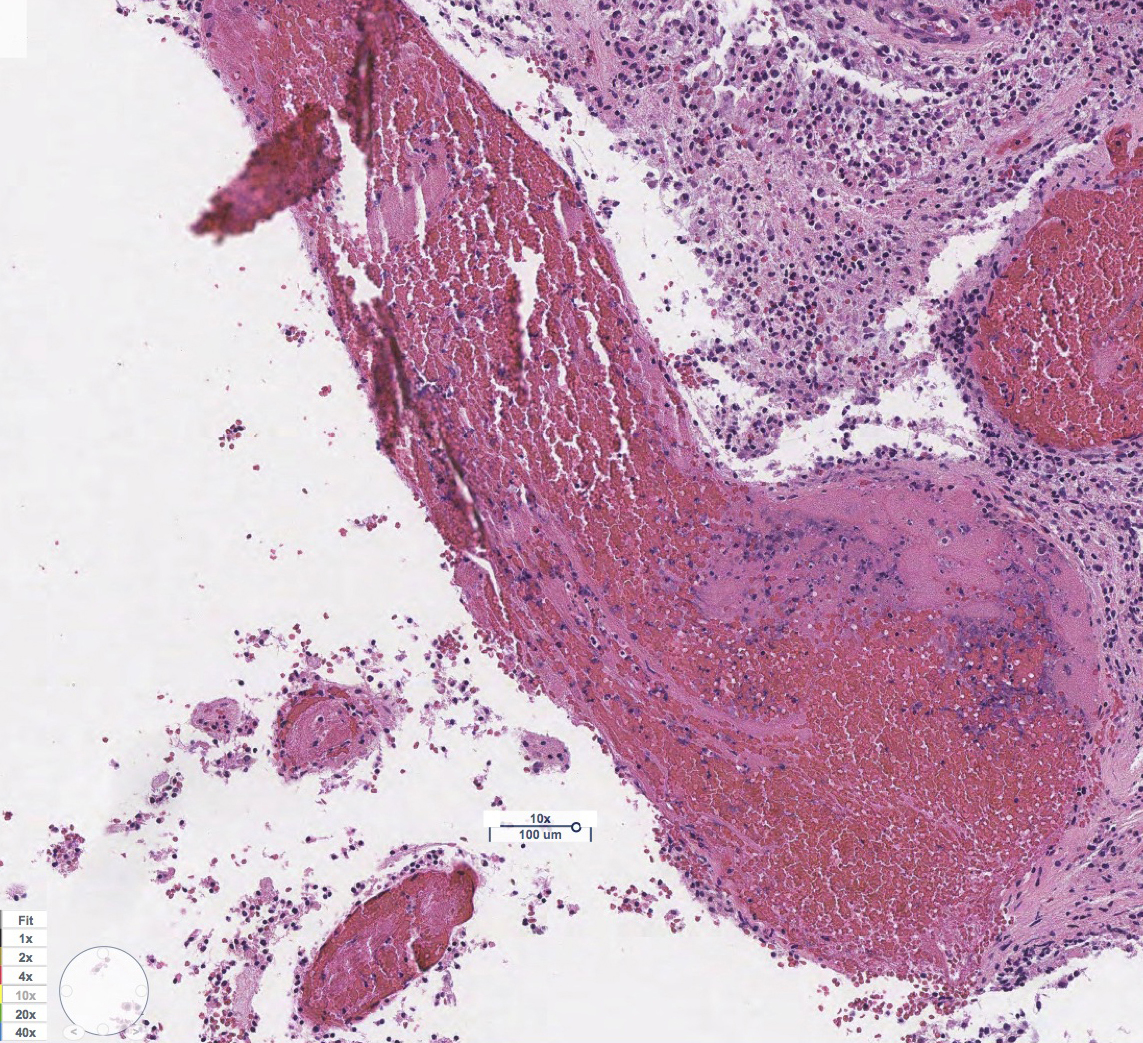 New research from the Department of Pathology was just published in Acta Neuropathologica. Led by a team of experts including Drs. Drew Pratt, Yelena Fudym, Sandra Camelo-Piragua, and Sriram Venneti, the study highlights H3K27M-mutant diffuse midline glioma with extensive intratumoral microthrombi in young adults with COVID-19.
New research from the Department of Pathology was just published in Acta Neuropathologica. Led by a team of experts including Drs. Drew Pratt, Yelena Fudym, Sandra Camelo-Piragua, and Sriram Venneti, the study highlights H3K27M-mutant diffuse midline glioma with extensive intratumoral microthrombi in young adults with COVID-19.
The study first examined the emergence of the novel coronavirus disease in 2019 and the unique challenges it presents for oncology patients. Experts analyzed the case of a 21-year-old woman who presented with headaches, blurry vision, and vomiting. Her neurologic examination showed no abnormalities, and the patient was diagnosed with tension-type headache. Two months later, she experienced a syncopal episode. Head CT demonstrated a large (4.3 cm) supratentorial thalamic mass causing obstructive hydrocephalus. She subsequently decompensated from herniation and underwent emergent ventricular drain placement. Post-operative head CT and MRI demonstrated successful drain placement, but exhibited marked hemorrhage in the tumor and ventricles, with a displacement of the septum pellucidum. The patient tested positive for SARS-CoV-2 by nasopharyngeal swab and exhibited classic findings of COVID-19-associated coagulopathy including elevated D-dimer levels, without changes in prothrombin or activated-partial-thromboplastin time. She exhibited no respiratory symptoms, and a chest radiograph demonstrated no evidence of lung disease.
 As Dr. Venneti describes, "The effect of COVID-19 on cancer patients has been enormous. Delays in treatment and access to care have had significant negative implications. However, how COVID-19 infection directly impacts the tumor micro-environment is not known. The brain has shown a unique susceptibility to strokes in COVID-19 infection. It is thought that the cytokine storm seen in some COVOD-19 patients results in blood clotting abnormalities that can cause strokes and bleeding within the brain."
As Dr. Venneti describes, "The effect of COVID-19 on cancer patients has been enormous. Delays in treatment and access to care have had significant negative implications. However, how COVID-19 infection directly impacts the tumor micro-environment is not known. The brain has shown a unique susceptibility to strokes in COVID-19 infection. It is thought that the cytokine storm seen in some COVOD-19 patients results in blood clotting abnormalities that can cause strokes and bleeding within the brain."
Ultimately, recent reports suggest a unique predisposition of the brain to thrombosis in COVID-19 infections attributed to a cytokine storm syndrome. Given the poor association between intratumoral microthrombi and overall prognosis in gliomas, our case raises a critical question concerning the impact of COVID-19-associated coagulopathy on tumor biology, the immune microenvironment, and, in this case, the patient’s clinical course. The case in question poses the hypothesis that COVID-19-associated coagulopathy could affect long-term tumor behavior and disease progression in cancer in a manner yet unrecognized.
"Surprisingly, [we] found similar micro clots and bleeding within a DIPG-like brain tumor in a young adult that negatively impacted the clinical course of this patient. These findings suggest that COVID-19 can cause changes within the tumor micro-environment and can potentially influence tumor biology," concludes Venneti.
The full publication in Acta Neuropathologica is accessible here.
 ON THE COVER
ON THE COVER
 ON THE COVER
ON THE COVER
 ON THE COVER
ON THE COVER
 ON THE COVER
ON THE COVER
 ON THE COVER
ON THE COVER
 ON THE COVER
ON THE COVER
 ON THE COVER
ON THE COVER
 ON THE COVER
ON THE COVER
 ON THE COVER
ON THE COVER
 ON THE COVER
ON THE COVER
 ON THE COVER
ON THE COVER
