

By Leslie Stainton | 12 July
 Patient Brenda Berky views results of her bone marrow biopsy on a monitor in the lab.
Patient Brenda Berky views results of her bone marrow biopsy on a monitor in the lab.
When Jeffrey Myers walks through University Hospital on his way to work, he often sees people waiting for appointments or trying to find their way to a clinic, and he’s reminded of why he does what he does. He’s grateful for the reminder because, as he puts it, “in pathology, it can be especially challenging to stay connected to our purpose—our why.” Lately, Myers, the A. James French Professor of Pathology, has become even more aware of how central patients are. It’s a given, of course, that patients are at the heart of health care. But in pathology, the sheer volume of work—and the fact that it mostly takes place at a remove from actual patients—can sometimes cloud the fact. U-M’s anatomic and clinical pathology labs conduct nearly six million tests a year. Every one of those tests is a person, says U-M pathologist Laura Cooling, “and I would hope we never forget the patient at the end of that blood specimen.” Cooling, who specializes in transfusion medicine, often works directly with patients, and she long ago recognized that “patients are infinite teachers.” It’s one reason she signed up to take part in the Department of Pathology’s new Patient and Family Advisory Council, or PFAC—a multidisciplinary initiative launched by Myers in 2016 with the aim of expanding and deepening the department’s engagement with patients.
"Patients are infinite teachers."
Myers and Cooling are among more than 40 faculty, staff, and technicians from the Department of Pathology who are part of the council—along with seven volunteer patient and family advisors. One of those advisors is Michele Mitchell, who co-chairs the council with Myers. A self-described “talker” with bright blonde hair and a ready laugh, Mitchell was treated at U-M for breast cancer in 2006 and says that after her cancer journey, she had a “burning desire to give back to this institution that, quite frankly, saved my life.” She leapt at the chance to join PFAC. The pathology council is one of nearly 30 Patient and Family Advisory Councils at U-M, all of them part of a system-wide effort to ensure that patients and their families stay at the heart of everything Michigan Medicine does. While the concept of patient-and family-centered care is now common throughout the United States—particularly in specialties like oncology and pediatrics, where families are often deeply involved in caring for loved ones—the idea of a pathology council is novel. It’s so novel, in fact, that last year when Myers took 22 members of PFAC to a national conference on patient-and family-centered care, people said to him, “Wait a minute! Pathologists—and people?” To which Myers cheerfully responds: “Why not?”
Like her fellow patient and family advisors in PFAC, Mitchell had almost no idea what pathologists did before joining the council. Even when she was undergoing her own cancer treatments, she never saw a pathology report, never talked to a pathologist. Fellow PFAC advisor Dennis Serras, also a cancer survivor, says the same. He never met a single pathologist during his care at U-M, despite the fact that “it was such a large part of my surgery and everything.” But since joining PFAC, pathology has become his favorite specialty. Even though pathologists are “off by themselves in their labs, and nobody knows about them,” Serras says, “patients and families need to know how important a role they play in their journey.” “We are the big black box,” says Cooling, who suspects most non-pathologists get their understanding of the field not from real-life experience but from forensic crime dramas on TV. Patients aren’t the only ones in the dark, she adds. Clinicians and medical students don’t always understand what takes place in the pathology labs, and that can make them uncomfortable talking to patients about pathology reports. Cooling hopes PFAC will help showcase “the breadth and opportunity of pathology in health care” and perhaps even help recruit medical students to the field. Like Myers, Cooling wants to see pathology play a larger role in patient care.To that end, she is overseeing one of PFAC’s key projects—a 20-minute video, slated for completion in early 2019, that takes viewers behind the scenes of Michigan Medicine’s pathology labs with 35-year-old Brenda Berky, a former leukemia patient now in remission. Berky was thrilled to volunteer for the project. She, too, knew nothing about pathology when she underwent treatment at U-M four years ago—except that people came into her hospital room two or three times a day to take blood from her when “I didn’t have much to give!” she recalls.“If I’d had a better understanding of what it was for, I probably wouldn’t have had such an attitude about it.”
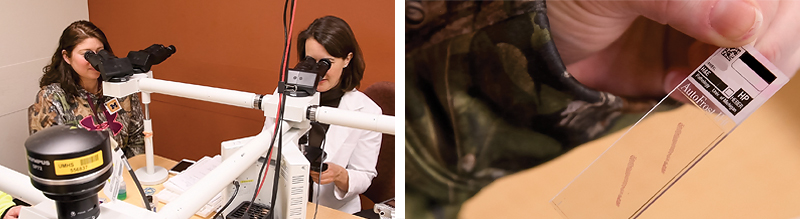 (left) Berky sits with Dr. Lauren Smith to view her slides at the multi-headed scope; (right) A slide containing Berky's tissue sample.The video tracks Berky during a series of follow-up visits to Michigan Medicine. Viewers can see her go through a blood draw and then walk her sample down to the pathology labs for analysis. Berky says that while filming the video, it brought tears to her eyes to see how concerned the lab technicians were about the patients whose specimens they were testing. “Just knowing that other people who have never met you care—that helps.” During one video session, Berky got to compare slides from her original diagnosis with her slides today. In the first slide, she remembers,“I was basically dying. And then I look at the next slide, and I realize that’s why I feel the way I do today, that’s why I’m here.” She hopes the PFAC video will help make new patients feel less afraid, in part by helping them see “that each time they come and take your blood, or do a bone marrow biopsy or a spinal tap, it isn’t for nothing. They have to do this to make you better.”
(left) Berky sits with Dr. Lauren Smith to view her slides at the multi-headed scope; (right) A slide containing Berky's tissue sample.The video tracks Berky during a series of follow-up visits to Michigan Medicine. Viewers can see her go through a blood draw and then walk her sample down to the pathology labs for analysis. Berky says that while filming the video, it brought tears to her eyes to see how concerned the lab technicians were about the patients whose specimens they were testing. “Just knowing that other people who have never met you care—that helps.” During one video session, Berky got to compare slides from her original diagnosis with her slides today. In the first slide, she remembers,“I was basically dying. And then I look at the next slide, and I realize that’s why I feel the way I do today, that’s why I’m here.” She hopes the PFAC video will help make new patients feel less afraid, in part by helping them see “that each time they come and take your blood, or do a bone marrow biopsy or a spinal tap, it isn’t for nothing. They have to do this to make you better.”
Shortly after she joined PFAC, Mitchell, too, got to see the original slides that led to her breast cancer diagnosis in 2006. She wept at the sight. People had told her at the time that her cancer, stage 1, was “no big deal.” But the slide told another story. Mitchell couldn’t believe how many cancer cells it held—a sight at once humbling and gratifying. She’s not sure she’d have wanted to see those cells at the start of her treatment, but she’s glad to have seen them later. “I wanted to see the enemy,” she says. “I wanted to see how big it was.” Not every patient is as curious as Mitchell, who likens herself to “a big old funnel.” But for those who are, information can be empowering.
Robyn Bishop, another PFAC advisor, recalls how bewildered she was 16 years ago when she gave birth to premature triplets who were rushed into the Neonatal Intensive Care Unit. Bishop had never spent much time in a healthcare setting, and she was overwhelmed. It’s why she’s especially admiring of a recent PFAC initiative, run by pediatric pathologist Raja Rabah, that puts pathologists in touch with families who’ve lost infants so that the families can get a more detailed understanding of their child’s autopsy report. These kinds of conversations can be difficult, but they’re crucial, says Myers. In his own practice, he’s found that the days when he has one-on-one talks with patients are his best days.“I don’t feel drained as a consequence of those conversations—I feel energized.” Patient conversations aren’t just “touchy-feely,” Myers emphasizes. They can help pathologists do a better job. Myers recalls one case where a conversation with a patient led him to go back to his colleagues at U-M and revisit their diagnosis. Having learned more from the patient about her medical history, Myers thought they may have misinterpreted her slides—and it turns out they had. “We have to get better at engaging patients further upstream in their interactions with the health system,” Myers believes. He envisions a day when pathologists confer up front with clinicians about the wisdom of even doing a biopsy in the first place, or of doing surgery. He can imagine pathologists meeting with patients after diagnosis to help them better understand the ramifications of their condition and make appropriate plans.
In all his years of shepherding children and later aging parents through Michigan Medicine, PFAC advisor Dale Perry never had any encounters with pathology—or at least that’s what he thought. “It turns out pathology touches everything,” he smiles. Perry joined PFAC with an eye toward giving back to the system that had helped his family so much, and now the field he once regarded as a “stealth specialty” is dear to his heart. He was especially “blown away” by a tour of U-M’s facilities last year. When he learned how many specimens pass through the labs annually, Perry gasped. The quantity alone—115,000 specimens, not including autopsies, in the anatomic pathology labs; 5.8 million tests in clinical pathology—was staggering. Even more stupefying was the thought that every one of those analyses had to be “of the very highest quality. People make life decisions based on the results of these tests.” A former journalist for the Detroit Free Press, Perry is using his communication skills to help launch one of PFAC’s most ambitious outreach projects, StoryCorps, aimed at capturing audio conversations that can illuminate the patient experience at U-M. The endeavor is part of the nationwide StoryCorps Legacy project, and Perry and his colleagues at U-M will receive on-site training from StoryCorps mentors on how to record, preserve, and disseminate patient stories. Although the specifics of the project are still in flux, Perry can imagine recording conversations between patients and their pathologists, for example, or among family members remembering what it was like to wait for a biopsy report. U-M’s StoryCorps recordings will be made available online to patients and their families, and stories collected during the program’s initial phase will be permanently filed at the Library of Congress. “People can’t always be present to tell their own stories, so we want to find a way to get their stories in front of people and to have those stories live forever,” Perry says.
 Dr. Jeffrey Myers and Patient Family Advisory Council Patient Chair, Michele Mitchell, hold a discussion about the PFAC initiative.
Dr. Jeffrey Myers and Patient Family Advisory Council Patient Chair, Michele Mitchell, hold a discussion about the PFAC initiative.
During monthly meetings of the council, PFAC members explore new ways to hear patient voices and build bridges. There’s talk of a more robust department website, a more informative online patient portal, increased bedside and clinical interactions between pathologists and patients, new spaces where these interactions can take place. In one pilot PFAC program, patients at the Cancer Center’s Multidisciplinary Lymphoma Clinic were given the option of talking with a pathologist. Sixteen patients did, and “they really loved it,” Myers says. “And the clinicians really loved it.” The program was so popular it’s now advertised on the clinic’s website. Myers acknowledges the challenges ahead. New financial models will have to be developed. Physician training will have to change as well, though perhaps not as much as one may think. The department’s impending move to U-M’s North Campus Research Complex, slated for later this year, is a big concern. Myers worries that when he and his colleagues are farther away from University Hospital, they’ll miss those random patient encounters that are so vital a reminder of their “why.” But council members are working to address that—and projects like StoryCorps and the PFAC video will do much to keep faculty and staff mindful of the patients they serve. As for Myers himself, who as a kid growing up in North Dakota dreamt of becoming a minister or social worker before opting to be a pathologist, PFAC is a dream come true. “I’ve believed for a long time that pathology can change the patient experience in very meaningful ways,” he grins. “To me that’s why we’re here.” The council, he adds, is “the thing that excites me most. I pinch myself every day that I’m able to do this.”